In the past, the diagnosis “inflamed dental nerve” was often a death sentence for a tooth. Extraction was the quick but final solution. Today, the tables have turned. Modern endodontics (the study of the tooth interior) is one of the most disciplined specialties in dentistry. Its sole goal: to preserve the natural tooth biologically. Because no implant is as good as the original.
However, horror stories still surround “root canal treatment.” We want to clear things up—with myths and outdated notions.
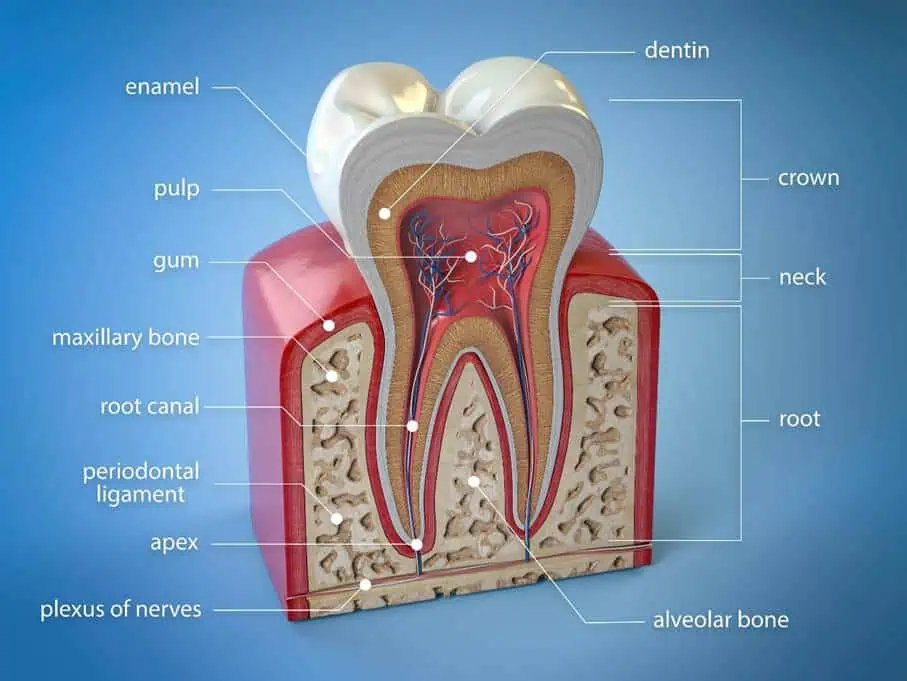
Why Does the Tooth Hurt at All?
To understand the treatment, it is worth looking beneath the hard shell.
- On the outside, enamel protects (the hardest substance in the human body).
- Beneath that lies the dentin.
- Inside is the pulp (often called the “dental nerve”). It is a highly complex tissue consisting of nerve fibers, blood vessels, and connective tissue.
When bacteria penetrate this protected chamber through deep decay or a crack, the tissue becomes inflamed (pulpitis). Since the tooth is hard and cannot expand, the inflammation creates enormous pressure—the typical throbbing toothache. If the tissue dies, bacteria can migrate into the jawbone and form painful abscesses there.
The Modern Process: High-Tech Instead of “Pulling the Nerve”
A root canal treatment today is a microsurgical procedure inside the tooth. The goal is not only pain relief, but sterility. Here is how a session proceeds according to current state of the art:
1. Absolute Isolation (Rubber Dam)
This is the most important step for long-term success. We place an elastic rubber sheet (rubber dam) around the tooth.
- The advantage: The tooth is isolated from the rest of the oral cavity. No saliva (full of bacteria) enters the tooth, and no rinsing solutions reach your mouth. You can breathe and swallow comfortably.
2. Looking into the Depths (Microscope)
Root canals are often hair-thin and curved. Many canal openings cannot be found with the naked eye. Under a dental microscope with up to 25× magnification, we can identify even hidden accessory canals that were often overlooked in the past and later led to renewed problems.
3. Electronic Measurement (Endometry)
Instead of relying solely on two-dimensional X-ray images as in the past, we measure the length of the root canals electronically. This is precise to the millimeter and spares you unnecessary radiation exposure.
4. 3D Cleaning and Disinfection
Using highly flexible nickel-titanium files that adapt to the curvature of the root, the infected tissue is removed. However, the chemistry is crucial: the canal is intensively rinsed and the rinsing solution is often activated using ultrasound. Only in this way can we reach the lateral niches that no file in the world can touch.
5. The Tight Seal
Once the tooth is bacteria-free, the hollow canal system is sealed three-dimensionally and bacteria-tight with a biocompatible natural material (gutta-percha).
Does It Hurt?
This is the most common question. The clear answer: No. In the case of acute inflammation, anesthesia may be more difficult at first (“hot tooth”), but with modern anesthetics and special injection techniques, the treatment is usually completely painless. Patients often even fall asleep during the longer cleaning procedure because the pain is finally gone.
Is the Effort Worth It?
Yes. A successfully root-treated tooth can last a lifetime with proper care. It remains firmly anchored in its natural position and provides a stable foundation for crowns or bridges. Trust expertise and technology with this complex topic—your tooth deserves this second chance.

